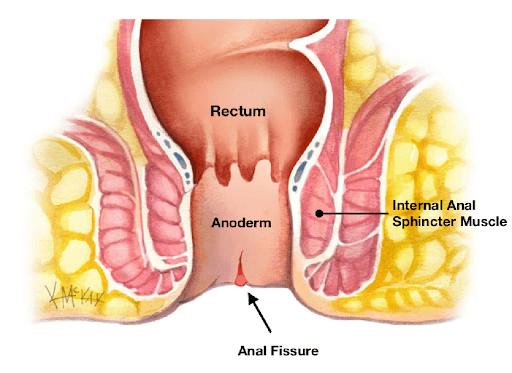
An anal fissure is a painful condition caused by a tear in the lining of the anus or anal canal, which is the opening through which stool passes out of the body. The anal lining is quite delicate. As a result, any cut or tear in this lining tissue can expose the muscle around the anus (anal sphincter), causing the patient to experience bleeding and painful bowel movements. Additionally, the damaged lining also causes the anal muscle to spasm, pulling the edges of the fissure apart during bowel movements.
A person is considered to have an acute anal fissure if it is recent or he or she has the condition for less than 6 weeks. The anal fissure is considered chronic if a patient has had it for more than 6 weeks or if it keeps coming back even after receiving treatment.
Since the symptoms of anal fissure overlap with complicated hemorrhoids, proctologists normally recommend visual exams like anoscopy and colonoscopy for a detailed study and to rule out other complications. In this blog, let us learn more about this condition, its causes, symptoms, treatment, and management.
Anal fissures: Are you at risk?
As discussed, anal fissures are tears that appear in the lining of the anal canal due to any trauma or injury to the anus. People suffering from constipation or explosive or ongoing episodes of diarrhea are highly prone to developing fissures. Passing hard or large stools, vaginal childbirth, insertion of foreign objects into the anus or anal sex are also possible reasons for the formation of fissures. Apart from trauma, fissures also form due to poor bowel habits, the presence of tight or spastic anal sphincter muscles, or scarring in the anorectal area. Anal fissures also form due to other medical conditions such as anal cancer, Crohn’s or ulcerative colitis, Leukemia, HIV, and certain STDs.
Fissures form in both men and women and can happen at any age. Although adults between the ages of 20 and 40 are at the highest risk of developing the condition, anal fissures are also formed in babies when they try to pass hardened stool. Experts note that generally, the risk of anal fissures goes down with increasing age. However, people who had fissures in the past are more likely to get them again in the future. To reduce the risk of recurrence, recovered patients must strictly adhere to the lifestyle changes recommended by their proctologist.
Symptoms to look out for
If a fissure has formed in the anal lining, you will experience the following symptoms-
- Painful bowel movements
- Pain sustaining for hours after the bowel movement
- Blood on the stool and toilet wipes
- Constipation
- Burning sensation in and around the anus
- Painful itch in and around the anus
- Visible crack or tear in or near the anus/anal canal
- Uncomfortable and frequent urination or inability to urinate
- Foul-smelling discharge from the anus
While some of the symptoms overlap with hemorrhoids, your proctology doctor may be able to identify the exact issue by listening to your symptoms themselves. So, do not hesitate to share your difficulties, without feeling embarrassed. Remember that the patient’s account is crucial in assessing the condition and receiving proper treatment.
Diagnosis, treatment, and prevention
If your proctologist suspects anal fissures, he can confirm it with the help of a physical examination of the anus and anal canal. For a thorough examination, your doctor may use an anoscopy for better visuals.
Generally, a visual exam is all it takes to confirm the cause of the anal fissure. However, if your proctologist suspects that something else triggered the fissure formation- like an inflammatory bowel disease- he may recommend additional tests such as sigmoidoscopy or colonoscopy. Both these tests involve the insertion of a long, flexible lighted tube into your anus for a detailed view of the lowest part of your bowel. The procedure will also confirm the presence of abnormal growths or inflammations if any.
If your anal fissure is not caused by other underlying conditions, your doctor may suggest taking steps to keep your stools soft and let the fissure heal on its own in the meantime. To aid the natural healing of the fissure, you will be put on a fiber-rich diet containing more fruits and vegetables. You will also have to take a fiber supplement or laxative to avoid constipation and the passing of hardened stool. Additionally, you will also have to drink more fluids and keep yourself hydrated.
Experts also recommend the use of sitz baths to help your fissure heal faster. Fill a sitz bath with warm water and sit in it for about 10-20 minutes several times throughout the day. There is no need for any soap or medication to be put into the water. Using a sitz bath after a bowel movement will help relieve the pain after passing stool.
If you have a chronic or recurring case of anal fissures, you will require medical intervention. Some of the common anal fissure treatment methods are discussed below-
- Topical Nitrates And Calcium Antagonist Medications
A prescription of 0.2% Glyceryl trinitrate (GTN) ointment is to be applied over the anal opening twice a day for 8 weeks. Sometimes, patients may experience headaches as a side effect of this medication due to systemic absorption and vasodilation. If so, your doctor may recommend applying Nifedipine 0.5% or diltiazem 2% ointment thrice daily around the anal opening.
- Botulinum Toxin (Botox)
Botox injections are seen to have a significant effect on anal fissure treatment. A combination of Botox and topical muscle relaxant treatment is used to reduce muscle spasms in the anal region due to fissure. This helps heal the anal fissure faster.
- Lateral Internal Sphincterotomy
If topical medications are not working, proctologists recommend surgical intervention. Earlier, doctors used to rely on anal dilation as the recommended treatment. However, this has been abandoned for the high risk of muscle injury causing anal incontinence.
Different surgical approaches are currently used.
Lateral Internal Sphincterotomy should be considered the last option because of the risk of incontinence. However, if this is performed by an expert proctologist that will cut only the small amount of muscle needed for the fissure to heal, the risk of incontinence is very low. The success rate is very high.
- Advancement Flaps.
- In this procedure the anal muscles are not cut. The flap consists of the skin and subcutaneous flap which is developed distally to the fissure. This surgery is also observed to have high healing rates.
Fissurectomy
Fissurectomy is a surgical procedure that involves excising the edges of the anal fissure, removing the granulation tissue, and excising any hypertrophied papilla or scar tissue. The resulting wound is either sutured or left open to heal naturally. Studies show that a combination of fissurectomy with Botox injections has a 93% healing rate.
Takeaway
Anal fissures are very common, especially in association with other digestive tract issues. To manage and prevent anal fissures from recurring, experts recommend eating a fiber-rich diet, drinking plenty of fluids, and practice healthy and hygienic bowel habits. If you suffer from constipation or hard stools, talk to your doctor and get a prescription laxative to soften your stools.
If you have any questions or concerns regarding anal fissures, book your appointment with Dr. Antonio Privitera, one of the best proctologists in the country for a comprehensive consultation.

