Hemorrhoids Treatment in Dubai
Table of Contents
- 1. What Are Hemorrhoids?
- 2. Symptoms of Hemorrhoids
- 3. It's Not Always Hemorrhoids: Differential Diagnosis
- 4. Red Flags: When You Need Urgent Evaluation
- 5. Internal vs External Hemorrhoids
- 6. Hemorrhoid Grading System
- 7. What Causes Hemorrhoids?
- 8. Treatment Options in Dubai
- 9. Recovery: What to Expect
- 10. What to Expect at Your First Visit
- 11. My Approach: What Sets This Practice Apart
- 12. Frequently Asked Questions
- 13. References and Medical Sources
Hemorrhoid treatment in Dubai requires accurate diagnosis and choosing the right technique for your specific condition. Most patients can be treated effectively with modern, minimally invasive procedures when managed by a specialist. I'm Professor Dr. Antonio Privitera, a consultant colorectal surgeon with fellowship training at the Mayo Clinic and in London, and European Board Certification in Colorectal Surgery. I specialize in the diagnosis and treatment of hemorrhoids and other anorectal conditions.
In my practice, I see patients every day who've delayed seeking care because of embarrassment or fear of surgery. The truth is straightforward: most hemorrhoids don't require surgery, and when they do, modern techniques have dramatically reduced pain and recovery time.
What matters most is accurate diagnosis because not all rectal bleeding or discomfort is caused by hemorrhoids and choosing treatment based on the grade and type of hemorrhoid you have, not marketing claims.
Professor Dr. Antonio Privitera Mayo Clinic & University of London Fellowship | FRCS | FASCRS
Discreet same-day assessment available. No referral required.
Medcare Discovery Gardens, Dubai
Here's what sets our approach apart:
- Accurate diagnosis first: We examine you properly (visual inspection, digital exam, anoscopy when needed) to confirm hemorrhoids and rule out other causes.
- Grade-based treatment: We match the treatment to your condition, not the other way around.
- Discreet, same-day assessment available: Privacy matters. We offer complete confidentiality across Dubai.
This guide explains everything you need to know about hemorrhoids, from symptoms and diagnosis to the full range of treatment options available in the UAE.
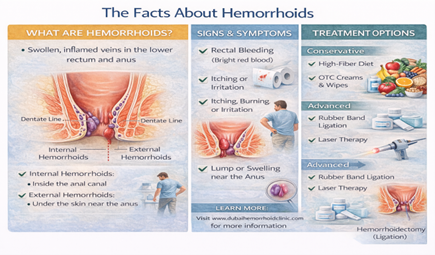
What Are Hemorrhoids?
Hemorrhoids (also called piles) are swollen blood vessels in the lower rectum and anal canal. Everyone has hemorrhoidal tissue these vascular cushions help with continence and sensation. Hemorrhoids become a problem when they enlarge, bleed, prolapse (come out of the anus), or cause pain.
There are two types:
- Internal hemorrhoids: Sit inside the rectum, above the dentate line. They typically don't hurt because they have no pain receptors they primarily bleed.
- External hemorrhoids: Are under the skin around the anus. These can be painful, especially if a clot forms (thrombosed external hemorrhoid).
Symptoms of Hemorrhoids: What You Might Notice
Hemorrhoid symptoms vary depending on whether they're internal or external. Typical experiences include:
- Bleeding: Bright red blood on toilet paper or in the bowl.
- A lump or swelling: A soft lump near the anus or a painful thrombosed clot.
- Itching or irritation: Caused by mucus discharge.
- Discomfort or pain: Especially with external or strangulated hemorrhoids.
Red Flags: Urgent Evaluation Needed
Seek medical care quickly if you experience: Heavy bleeding, dizziness, severe constant pain, fever with swelling, or unexplained weight loss.
Internal vs External Hemorrhoids: Why the Difference Matters
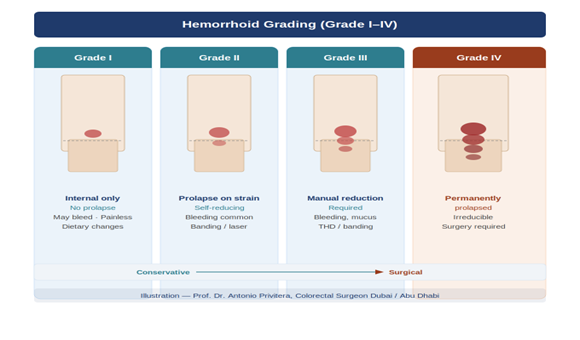
Hemorrhoid Grading System
Grade I: Bleed but don't prolapse.
Grade II: Prolapse during straining but go back in on their own.
Grade III: Prolapse and require manual reduction (pushing back in).
Grade IV: Permanently prolapsed and cannot be pushed back inside.
Why grading matters: Different treatments work for different grades. A Grade IV usually requires surgery, while Grade I often responds to lifestyle changes. The safest approach is grade-based treatment selection.
What Causes Hemorrhoids? (And Dubai-Specific Risk Factors)
Hemorrhoids develop when there's increased pressure on the blood vessels in the rectum and anus. Common causes include:
- Straining during bowel movements: Chronic constipation and hard stools are the most common culprits.
- Prolonged sitting: Especially on the toilet. In Dubai, I see this frequently in office workers who sit 10 to12 hours a day.
- Low-fiber diet: Many expatriates in the UAE eat less fiber than in their home countries.
- Dehydration: Dubai's heat and air conditioning lead to harder stools. Aim for 2.5 to 3 liters of water daily.
- Pregnancy and childbirth: Increased pressure on pelvic veins and hormonal changes.
In my practice, I see patterns: long office hours, dehydration from coffee/tea, eating out frequently (low fiber), and delayed care due to busy schedules.
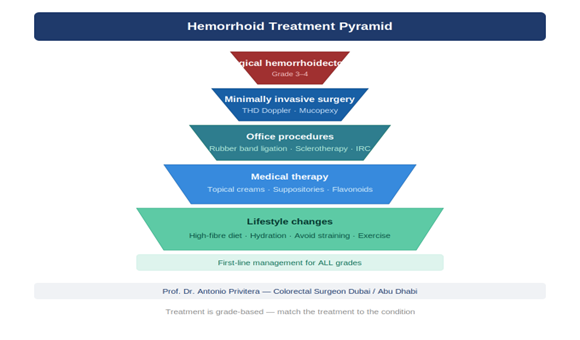
Treatment Options in Dubai: From Conservative Care to Surgery
Treatment depends on the type and grade of hemorrhoid. Here is my approach, from least invasive to most invasive.
Conservative Treatment (First-Line)
For Grade I and early Grade II, lifestyle changes are often all you need. This includes a fiber target of 25 to 35 grams daily and proper hydration.
Office Procedures (Grade I–II)
I place a small band around the base of an internal hemorrhoid. It shrinks and falls off within a week. Best for Grade I and II.
Sclerotherapy & Infrared Coagulation:Chemical injections or light energy to shrink early-grade hemorrhoids.
Minimally Invasive Operating Room Procedures
Laser fiber shrinks the hemorrhoid from inside. Recovery is 3 to 7 days. Ideal for Grade II and III.
THD (Transanal Hemorrhoidal Dearterialization):Using Doppler ultrasound to tie off arteries. No tissue is cut, meaning less pain and 5 to10 days recovery.
Surgical Treatment: Hemorrhoidectomy
For Grade 4 hemorrhoids or large mixed cases, surgical removal is the most definitive cure with the lowest recurrence rate.
Recovery & What to Expect
Recovery depends on the treatment: Office procedures require 1 to 2 days, while hemorrhoid recovery takes 7 to14 days for desk work.
First Visit: We perform a visual inspection, digital rectal exam, and anoscopy. If there are red flags, I may recommend a colonoscopy to rule out other issues.
My Approach: What Sets This Practice Apart
I believe in matching the treatment to your specific situation. If you were my family member, I'd tell you: don't be embarrassed, get a proper exam, and don't rush into expensive surgery if a simpler procedure works.
I check for skin tags indicating a previous thrombosed hemorrhoid emergency and look for the whole picture, ensuring you get a grade-based plan that fits your Dubai lifestyle.
Frequently Asked Questions
No. While common, other conditions like fissures, fistulas, polyps, IBD, and colorectal cancer also cause bleeding. If you're over 40 or have a family history of cancer, an examination is essential.
It depends. If you're 40 or older and haven't been screened, I recommend it even if hemorrhoids are present. In the UAE, screening typically begins at age 40 to rule out polyps or cancer coexisting with hemorrhoids.
Grade I can often resolve with diet. Grade II and III usually require intervention (like banding or laser) because structural prolapse doesn't correct itself with lifestyle changes alone.
- Grade I-II: Banding or Sclerotherapy
- Grade II-III: Laser or THD
- Grade IV: Hemorrhoidectomy
The safest approach is matching treatment to your specific anatomy and grade.
It is less painful than traditional surgery, but not painless. "Scar-free" is misleading as all procedures create a healing response. It's a great tool but marketing often overpromises.
A thrombosed external hemorrhoid is a sudden, painful clot. If seen within 48-72 hours, I can remove it under local anesthesia for immediate relief. Otherwise, it gradually dissolves on its own.
The first week is uncomfortable, especially during bowel movements. However, modern pain management and stool softeners make it much more tolerable than in the past. Most are back to light activity in 7-14 days.
No, they don't turn into cancer. But since they share symptoms (bleeding), we must examine you properly to ensure an early cancer isn't missed.
Yes, due to pelvic pressure and hormonal changes. Most improve after delivery. We usually postpone surgical procedures until after breastfeeding.
- High-fiber fruits (berries, pears)
- Vegetables (broccoli, leafy greens)
- Whole grains and Legumes
- 2.5–3 liters of water daily
Yes. Prolonged sitting—especially on the toilet—increases pressure. Take breaks every hour and keep toilet time under 5 minutes.
Yes. Walking, swimming, and yoga are great. Avoid heavy squats or deadlifts until symptoms improve.
- Banding: 1-2 days
- Laser/THD: 3-7 days (desk jobs)
- Hemorrhoidectomy: 7-14 days (desk jobs)
Hemorrhoidectomy has the lowest recurrence rate. Maintaining high fiber and good hydration is the best way to prevent them from returning.
It's a 1-2 minute exam using a small lighted scope. You'll feel pressure but no pain. It is essential for an accurate internal diagnosis.
Not for office procedures (banding). For surgery or laser under sedation, you'll need to fast for 6-8 hours.
Yes. Just stay well-hydrated and bring stool softeners, as airplane cabins are very dry and sitting for long periods can be uncomfortable.
Most medically necessary treatments are covered by UAE insurance. We can help check your specific policy coverage before starting.
Yes. All consultations and examinations are completely private and confidential.
Look for fellowship-trained colorectal surgeons with board certification who offer the full spectrum of treatments, not just one technique.
References and Medical Sources
This article is based on current medical evidence and clinical practice guidelines:
- UAE Colorectal Cancer Screening Guidelines – Abu Dhabi Department of Health recommends screening starting at age 40 for average-risk individuals. Abu Dhabi Public Health Center – Colorectal Cancer Program
- Cleveland Clinic Abu Dhabi – Colorectal Cancer Screening Guidelines - Local clinical protocols for UAE population. CCAD Screening Guidelines
- Thrombosed External Hemorrhoids Treatment – Evidence for 48–72 hour intervention window. Greenspon J, Williams SB, Young HA, Orkin BA. Thrombosed external hemorrhoids: outcome after conservative or surgical management. Dis Colon Rectum. 2004;47(9):1493-8. PubMed Source
- Transanal Hemorrhoidal Dearterialization (THD) Outcomes – Success rates for Grade II–III hemorrhoids. Ratto C, Giordano P, Donisi L, et al. Transanal haemorrhoidal dearterialisation (THD) for haemorrhoidal disease: a single-centre study on 1000 consecutive cases. Colorectal Dis. 2017;19(8):750-756. PubMed Source
- American Society of Colon and Rectal Surgeons (ASCRS) – Clinical Practice Guidelines for the Management of Hemorrhoids. Davis BR, Lee-Kong SA, Migaly J, Feingold DL, Steele SR. Dis Colon Rectum. 2018;61(3):284-292. PubMed Source
- Rubber Band Ligation Effectiveness – Long-term outcomes for hemorrhoid banding. Shanmugam V, Thaha MA, Rabindranath KS, et al. Rubber band ligation versus excisional haemorrhoidectomy for haemorrhoids. Cochrane Database Syst Rev. 2005;(3):CD005034. Cochrane Library Source
Medical Review: This content was written and reviewed by Professor Dr. Antonio Privitera, Consultant Colorectal Surgeon, with fellowship training at the Mayo Clinic (USA) and Royal College of Surgeons (UK), and European Board Certification in Colorectal Surgery.
Locations and Booking
I see patients at multiple locations across Dubai. For specific clinic addresses and to confirm current availability at each location, please contact us directly.
If you are experiencing hemorrhoid symptoms, early assessment can help prevent complications and guide you toward the most effective treatment option.
Schedule a Discreet Consultation
If you're experiencing hemorrhoid symptoms bleeding, discomfort, prolapse, or itching I'm here to help. The first step is an accurate diagnosis, and together we'll develop a treatment plan tailored to your grade and lifestyle.
Same-day and next-day appointments are often available. All consultations are private and confidential.
Professor Dr. Antonio Privitera
Consultant Colorectal Surgeon
Fellowship Training: Mayo Clinic | Royal College of Surgeons (UK)
European Board Certified in Colorectal Surgery
About the Author

Dr. Privitera is the only surgeon in the world with both a Mayo Clinic (Rochester, USA) and University of London Colorectal Surgery Fellowship. He completed an advanced laparoscopic and robotic fellowship in Seoul, South Korea.
He previously served as Lead Colorectal Surgeon at Tawam Hospital–Johns Hopkins Abu Dhabi and Associate Professor at UAE University.
He is a Fellow of the American Society of Colon and Rectal Surgery (FASCRS), Fellow of the Royal College of Surgeons of England (FRCS), and author of over 70 peer-reviewed publications. He also served as General Secretary of the Emirates Society of Colon and Rectal Surgery (2021–2024).
He practices across Dubai and Abu Dhabi.
by Dr. Antonio Privitera — Last reviewed: March 2026
