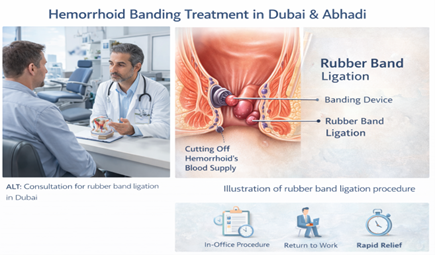
What It Is
Banding, laser, and THD for hemorrhoids in Dubai each suit different grades and patient needs. Choosing the right treatment depends on accurate diagnosis, anatomy, and symptom severity. For a full overview of the condition before exploring specific treatments, see our hemorrhoid treatment in Dubai.
office procedure for internal hemorrhoids. I place a small rubber band around the base of an internal hemorrhoid using a specialized instrument. The band cuts off blood supply. Within 5-10 days, the hemorrhoid withers and falls off (you usually don’t notice when this happens—it passes during a bowel movement).
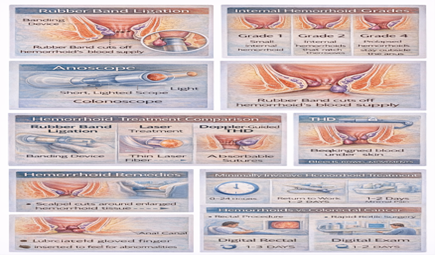
How It Works
The procedure takes 5-10 minutes and requires no anesthesia. Internal hemorrhoids have no pain receptors, so you feel only mild pressure or a sensation of fullness. I can typically band 1-2 hemorrhoids per session. If you have multiple hemorrhoids, you may need 2-3 sessions spaced 4-6 weeks apart.
Best For:
- Grade I hemorrhoids (bleed but don’t prolapse)
- Grade II hemorrhoids (prolapse during straining but go back in automatically)
- Small Grade III hemorrhoids (prolapse and require manual reduction)
Not Suitable For:
- Grade III with large external component (banding only treats internal hemorrhoids)
- Grade IV hemorrhoids (permanently prolapsed)
- Hemorrhoids too close to the dentate line (the band would be painful)
Recovery:
- Day 1: Mild discomfort, feeling of fullness or pressure. Take paracetamol if needed.
- Day 2-7: Most patients feel normal. The banded hemorrhoid is falling off (you usually don’t notice).
- Avoid: Heavy lifting for 3-5 days, straining during bowel movements
Most patients return to work the next day or within 1-2 days.
Success Rate:
Clinical studies show good effectiveness for appropriate grades. The key is patient selection—banding works excellently for Grade I-II but higher recurrence rates for Grade III-IV.
Recurrence: Variable depending on grade and whether lifestyle changes are maintained. Grade I-II patients who maintain high fiber diet and good bowel habits have low recurrence. Grade III patients may experience recurrence and need repeat treatment.
Advantages:
- ✅ Done in office (no operating room, no anesthesia)
- ✅ Minimal downtime (back to work next day)
- ✅ Very low risk
- ✅ Lowest cost
- ✅ Can repeat if needed
Disadvantages:
- ❌ Only treats internal hemorrhoids (not external)
- ❌ Not effective for Grade III-IV
- ❌ May require multiple sessions
- ❌ Moderate recurrence rate for Grade II-III
My Experience:
I perform banding regularly in my Dubai clinics. When grade is appropriate (I-II), patients are usually very satisfied—minimal discomfort, back to normal quickly, and symptoms resolve. The problems arise when banding is attempted on Grade III-IV hemorrhoids where it’s simply not the right tool for the job.
Laser Hemorrhoidoplasty: The Marketed “Painless” Option
Experiencing symptoms like these? A discreet same-day specialist assessment is available across Dubai.
WhatsApp: +971 55 318 8469 | Phone: +971 55 318 8469
Medcare Discovery Gardens (Dubai)
What It Is
Laser hemorrhoidoplasty (LHP) involves inserting a laser fiber into the hemorrhoid tissue and delivering controlled energy. This shrinks the hemorrhoid from the inside by coagulating blood vessels and causing fibrosis (scarring).
How It Works
Done in an operating room under sedation or spinal anesthesia. The procedure takes 20-30 minutes. The laser fiber is inserted into each hemorrhoid through a small puncture, energy is delivered for several seconds per hemorrhoid, and the fiber is withdrawn. No tissue is cut away—the hemorrhoid shrinks over the following weeks.
Best For:
- Grade II internal hemorrhoids (especially if banding has failed or patient prefers single-session treatment)
- Grade III internal hemorrhoids (without significant external component)
Not Suitable For:
- Grade I hemorrhoids (unnecessarily invasive and expensive—banding works just as well)
- Grade IV hemorrhoids (tissue is too prolapsed for laser alone to be effective)
- Large external hemorrhoids (laser targets internal tissue only)
Recovery:
Reality check: Laser is marketed as “painless” and “no downtime,” but this oversells the reality.
- Day 1-3: Moderate discomfort, managed with oral pain medication.
You’ll need stool softeners.
- Day 3-7: Gradual improvement. Most return to desk work by day 5-7.
- Week 2-3: Full recovery, though you’ll need to avoid heavy lifting for 2 weeks.
You will have pain—it’s less than hemorrhoidectomy (traditional surgery), but it’s not “painless.”
Success Rate:
Studies show good short-term results for Grade II-III internal hemorrhoids. Long-term data is more limited compared to banding or THD, as laser for hemorrhoids is newer.
Recurrence: Moderate. Some patients experience symptom recurrence after 1-3 years, though less commonly than with banding.
Advantages:
- ✅ Single session (no repeat appointments)
- ✅ Less pain than traditional hemorrhoidectomy
- ✅ Good for Grade II-III internal hemorrhoids
- ✅ Faster recovery than hemorrhoidectomy
Disadvantages:
- ❌ Overhyped marketing creates unrealistic expectations (“painless,” “no downtime”)
- ❌ Expensive (AED 15,000-25,000 in Dubai)
- ❌ Doesn’t treat external component
- ❌ Not effective for Grade IV
- ❌ Moderate recurrence rates
- ❌ Less long-term data than older procedures
My Honest Assessment:
Laser is a legitimate option for Grade II-III internal hemorrhoids, especially if you want a single-session treatment and banding has failed or isn’t suitable. However, be skeptical of clinics that push laser for everyone regardless of grade.
Red flags:
- Clinic recommends laser for Grade I hemorrhoids (banding is simpler and equally effective)
- Clinic claims laser is “completely painless” (it’s not)
- Clinic only offers laser and doesn’t perform banding or THD (suggests financial motivation, not clinical judgment)
Laser is a tool, not a miracle. It works well for the right patient but is often oversold.
THD (Transanal Hemorrhoidal Dearterialization): The Most Comprehensive Option
What It Is
THD, also called HAL-RAR (Hemorrhoidal Artery Ligation with Recto-Anal Repair), is a minimally invasive surgical procedure that addresses hemorrhoids by:
1. Dearterialization: Using Doppler ultrasound, I identify and ligate (tie off) the arteries feeding blood to the hemorrhoids
2. Mucopexy (RAR): I lift and stitch the prolapsed hemorrhoidal tissue back into its normal anatomical position
How It Works
Done in an operating room under spinal or general anesthesia. Takes 45-60 minutes. A specialized proctoscope with Doppler probe is inserted. I identify 4-6 hemorrhoidal arteries and ligate them with absorbable sutures. Then I perform mucopexy—lifting the prolapsed tissue and stitching it back to the rectal wall. No hemorrhoidal tissue is excised (cut away).
Best For:
- Grade II-III internal hemorrhoids (excellent results)
- Select Grade IV (without large external component)
- Patients who’ve failed banding or laser
- Patients who want low recurrence risk
Not Suitable For:
- Grade IV with large external component (external tissue won’t be addressed—hemorrhoidectomy is better)
- Large skin tags (THD doesn’t remove these)
Recovery:
THD is less painful than hemorrhoidectomy because no tissue is cut away.
However, it’s more invasive than laser.
- Day 1-5: Moderate discomfort, managed with oral pain medication and stool softeners. Most patients rest at home.
- Day 5-10: Gradual improvement. Most return to desk work around day 7-10.
- Week 2-4: Full recovery. Avoid heavy lifting for 2-3 weeks.
Success Rate:
Clinical studies show good long-term outcomes for Grade II-III hemorrhoids. One large study of 1,000 patients showed high patient satisfaction with low recurrence at 2-3 years.
Recurrence: Low compared to other minimally invasive procedures. THD addresses both blood supply and anatomical prolapse, which is why it has better durability.
Reference: Ratto C, Giordano P, Donisi L, et al. Transanal haemorrhoidal dearterialisation (THD) for haemorrhoidal disease: a single-centre study on 1000 consecutive cases. Colorectal Dis. 2017;19(8):750-756. PubMed
Advantages:
- ✅ Addresses both blood supply and prolapse (more comprehensive)
- ✅ Low recurrence rates
- ✅ Suitable for Grade III (where banding often fails)
- ✅ Less pain than hemorrhoidectomy
- ✅ Preserves hemorrhoidal tissue (maintains continence)
Disadvantages:
- ❌ Expensive (AED 18,000-30,000 in Dubai)
- ❌ Requires operating room and anesthesia
- ❌ Longer recovery than banding (5-10 days off work)
- ❌ Doesn’t treat large external components
- ❌ Requires specialized equipment and training (not all surgeons perform it)
My Experience:
THD is my preferred option for Grade III internal hemorrhoids and for Grade II patients who want definitive, low-recurrence treatment. The Doppler technology ensures I’m ligating the correct arteries, and the mucopexy restores anatomy—this combination gives excellent long-term results.
However, THD isn’t necessary for Grade I-II that respond to banding, and it won’t fix Grade IV with large external components (those need hemorrhoidectomy).
Which Treatment for Which Grade?
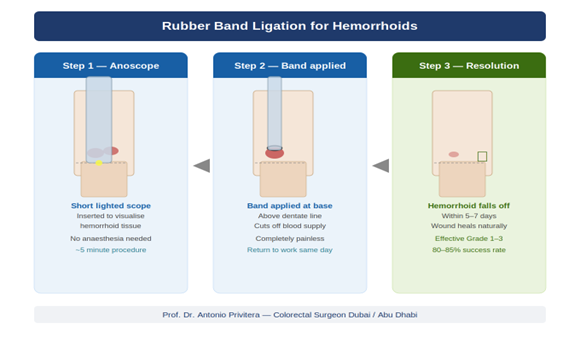
Here’s my clinical approach:
Grade I (Bleed but don’t prolapse):
- First-line: Conservative treatment (fiber, hydration, bowel habits)
- If bleeding persists: Rubber band ligation
- Avoid: Laser, THD (unnecessary and expensive)
Grade II (Prolapse during straining, go back automatically):
- First-line: Rubber band ligation
- If banding fails or patient prefers single-session: Laser or THD
- Consider THD if: Patient wants lowest recurrence risk and
doesn’t mind cost/recovery
Grade III (Require manual reduction):
- First-line: THD (best long-term results)
- Alternative: Laser (if internal only, no external component)
- Avoid: Banding alone (often insufficient for Grade III)
- If large external component: Consider hemorrhoidectomy
Grade IV (Permanently prolapsed, can’t be reduced):
- First-line: Hemorrhoidectomy (surgical excision)
- Consider THD only if: Minimal external component and patient
understands limitations
- Avoid: Banding, laser (won’t work for Grade IV)
Recovery Time: What to Expect
Banding:
- Time off work: 1-2 days (many return next day)
- Pain medication needed: Usually just paracetamol, if anything
- Restrictions: Avoid heavy lifting 3-5 days
- Full recovery: 1 week
Laser:
- Time off work: 3-7 days (desk jobs), 7-10 days (physical work)
- Pain medication needed: Oral pain medication for 3-5 days
- Restrictions: Avoid heavy lifting 2 weeks
- Full recovery: 2-3 weeks
THD:
- Time off work: 5-10 days (desk jobs), 10-14 days (physical work)
- Pain medication needed: Oral pain medication for 5-7 days
- Restrictions: Avoid heavy lifting 2-3 weeks
- Full recovery: 3-4 weeks
All three procedures require:
- Stool softeners to keep bowel movements comfortable
- High-fiber diet and hydration
- Sitz baths (warm water) 2-3 times daily
- Avoiding straining
If symptoms persist or are not improving, a specialist assessment in Dubai can help determine the most appropriate treatment.
Cost Considerations in Dubai
Cost varies by facility, surgeon experience, and whether insurance
covers the procedure.
Approximate Costs (Dubai):
Rubber Band Ligation:
- Per session: AED 1,500-3,000
- Total (2-3 sessions): AED 3,000-9,000
- Usually covered by insurance: Yes (medically necessary)
Laser Hemorrhoidoplasty:
- Single procedure: AED 15,000-25,000
- Insurance coverage: Variable (some insurers cover, some consider it elective)
THD (HAL-RAR):
- Single procedure: AED 18,000-30,000
- Insurance coverage: Usually yes if medically indicated (Grade III-IV)
Cost-Benefit Analysis:
For Grade I-II: Banding is most cost-effective. Paying AED 15,000-25,000 for laser when banding costs AED 1,500-3,000 and has similar success rates doesn’t make financial sense.
For Grade III: THD’s higher upfront cost is justified by lower recurrence rates. Paying AED 20,000 once is better than paying for repeated banding sessions (AED 3,000 × 3-4 times over years) plus eventual THD anyway.
Insurance considerations: Always check with your insurer before proceeding. Most cover medically necessary procedures (banding for Grade I-II, THD or laser for Grade III), but some consider laser “cosmetic” or “experimental” and deny coverage.
How to Decide: Questions to Ask Your Surgeon
When consulting about treatment, ask:
1. “What grade are my hemorrhoids?”
If the surgeon hasn’t examined you (anoscopy) and doesn’t tell you the grade, that’s a red flag. Treatment should match grade.
2. “Do I have internal only, or do I have external hemorrhoids too?”
Banding, laser, and THD only treat internal hemorrhoids. If you have significant external component, you may need hemorrhoidectomy or combined approach.
3. “Why are you recommending this specific treatment for my grade?”
The surgeon should explain how the treatment matches your anatomy. If they say “laser is the best” without explaining why it’s best for your specific grade, be skeptical.
4. “What are the success rates and recurrence rates for my grade?”
Ask for evidence. Banding has excellent success for Grade I-II. THD has better long-term results for Grade III. Laser sits in between.
5. “Do you perform all three procedures?”
If a surgeon only offers one option (especially laser), they have financial motivation to recommend it for everyone. A surgeon who performs banding, laser, THD, and hemorrhoidectomy will choose based on your anatomy, not their equipment.
6. “What will this cost, and will my insurance cover it?”
Get cost estimates upfront and confirm insurance coverage before proceeding.
My Approach: Matching Treatment to Anatomy
In my practice across Dubai, here’s how I approach
hemorrhoid treatment:
Step 1: Proper examination (anoscopy) to grade the hemorrhoids and identify internal vs external components.
Step 2: Match treatment to grade:
- Grade I-II → Start with conservative care, then banding if needed
- Grade III → THD (or laser if patient prefers)
- Grade IV → Hemorrhoidectomy
Step 3: Discuss options honestly:
- I explain what each procedure can and cannot do
- I tell patients when banding is sufficient (even though laser is more expensive)
- I tell patients when hemorrhoidectomy is necessary (even though THD is easier to recover from)
What I DON’T do:
- Push laser as “the latest technology” for Grade I hemorrhoids when banding works just as well
- Recommend expensive procedures when simple conservative care might work
- Claim any procedure is “painless” or “no downtime” (they have some discomfort and recovery)
The goal is the right treatment for your specific anatomy, not the most expensive equipment I happen to own.
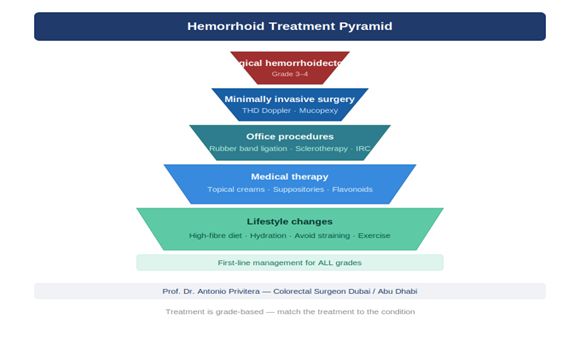
This article is written and reviewed by Prof. Dr Antonio Privitera, consultant colorectal surgeon with fellowship training at Mayo Clinic (USA) and the Royal College of Surgeons (UK), specializing in hemorrhoid diagnosis and minimally invasive treatment.
Frequently Asked Questions
1. Can I just go straight to THD instead of trying banding first?
If you have Grade III hemorrhoids, yes—THD is appropriate first-line treatment. But if you have Grade I-II, banding is simpler, cheaper, and equally effective. There’s no advantage to jumping to THD for early grades.
2. My clinic says laser is “the new standard.” Is that true?
No. Laser is a tool for certain situations, but it’s not automatically better than banding or THD. Calling it “the new standard” is marketing, not medicine. The standard approach is matching treatment to hemorrhoid grade.
3. Will insurance cover laser if I have Grade III hemorrhoids?
Possibly, but check with your insurer first. Some insurers cover laser for Grade III as medically necessary, while others consider it elective and deny coverage. THD is more consistently covered for Grade III.
4. If banding doesn’t work, should I try more banding sessions or
move to laser/THD?
Depends on your grade. For Grade II, trying 2-3 banding sessions is reasonable. If still symptomatic, move to laser or THD. For Grade III, if banding fails once, I usually recommend moving to THD rather than repeating banding multiple times.
5. Can I do banding and then THD later if needed?
Yes. Banding doesn’t preclude future THD or hemorrhoidectomy. Many patients with Grade II-III try banding first, and if it doesn’t provide lasting relief, we proceed to THD.
6. Which has the lowest recurrence: banding, laser, or THD?
THD has the lowest recurrence for Grade II-III hemorrhoids, followed by laser, then banding. However, “recurrence” depends partly on grade—banding has low recurrence for Grade I-II, but higher
recurrence for Grade III because banding isn’t designed for advanced prolapse.
7. Can I fly after these procedures?
After banding: Usually yes, even next day (though long flights may be uncomfortable)
After laser: Wait 5-7 days
After THD: Wait 7-10 days
8. Will I need to take time off work?
Banding: 1-2 days or less
Laser: 3-7 days (desk job), up to 10 days (physical work)
THD: 5-10 days (desk job), 10-14 days (physical work)
9. What if I have both internal and external hemorrhoids?
Banding, laser, and THD primarily treat internal hemorrhoids. If you have significant external hemorrhoids or skin tags, you may need: Banding/laser/THD for internal + separate excision of external components, or Hemorrhoidectomy (treats both internal and external at once)
10. How do I know if a clinic is just trying to sell me expensive
treatment?
Red flags:
Recommends laser for Grade I-II without trying banding first Claims one treatment is “best” for everyone regardless of grade
Only offers one type of procedure
Pushes treatment without proper examination (anoscopy)
Makes unrealistic promises (“painless,” “permanent cure,” “no downtime”)
Choose a surgeon who performs multiple procedures and chooses based on your anatomy, not their equipment.
References and Medical Sources
This comparison is based on current medical evidence:
1. Rubber Band Ligation Effectiveness – Cochrane review comparing banding to surgery.
Shanmugam V, Thaha MA, Rabindranath KS, Campbell KL, Steele RJ, Loudon MA. Rubber band ligation versus excisional haemorrhoidectomy for haemorrhoids. Cochrane Database Syst Rev. 2005;(3):CD005034. PubMed
2. THD Long-Term Outcomes – Large study showing effectiveness.
Ratto C, Giordano P, Donisi L, et al. Transanal haemorrhoidal dearterialisation (THD) for haemorrhoidal disease: a single-centre study on 1000 consecutive cases. Colorectal Dis. 2017;19(8):750-756. PubMed
3. American Society of Colon and Rectal Surgeons Guidelines –
Evidence-based treatment recommendations. Davis BR, Lee-Kong SA, Migaly J, Feingold DL, Steele SR. The American Society of Colon and Rectal Surgeons Clinical Practice Guidelines for the Management of Hemorrhoids. Dis Colon Rectum. 2018;61(3):284-292 PubMed
4. Laser Hemorrhoidoplasty Review – Current evidence and outcomes.
Maloku H, Gashi Z, Lazovic R, Islami H, Juniku-Shkololli A. Laser Hemorrhoidoplasty Procedure vs Open Surgical Hemorrhoidectomy: a Trial Comparing 2 Treatments. JAMA Surg. 2015;150(10):931-936. PubMed
Medical Review: This content was written and reviewed by Professor training at the Mayo Clinic and Royal College of Surgeons (UK), and European Board Certification in Colorectal Surgery.
Get Honest Assessment and Grade-Based Treatment Recommendation
No sales pitch. Just honest evaluation of what will work best for your specific hemorrhoid grade.
📱 WhatsApp: +971 55 318 8469
📞 Phone: +971 55 318 8469
🌐 Book Online:
Dubai Locations:
- Medcare Medical Centre, Discovery Gardens
- Medcare Women and Children Hospital
- Medcare Royal Specialty Hospital
- Clemenceau Medical Centre
- Aster Hospital, Qusais
I perform banding, laser, THD, and hemorrhoidectomy—so I recommend based on your anatomy, not my equipment.
Professor Dr. Antonio Privitera
Fellowship Training: Mayo Clinic | Royal College of Surgeons (UK)
European Board Certified in Colorectal Surgery