Early hemorrhoid symptoms in Dubai are often overlooked, but recognising them early can lead to simpler and more effective treatment. Prompt diagnosis helps prevent progression and avoids unnecessary suffering.
I am Professor Dr. Antonio Privitera, a consultant colorectal surgeon with fellowship training at the Mayo Clinic and the Royal College of Surgeons in London, and European Board Certification in Colorectal Surgery. I see patients daily across Dubai who have lived with hemorrhoid symptoms for weeks or months before seeking help.
The most important thing I can tell you is this: most hemorrhoid symptoms are straightforward to diagnose and treat. For a complete picture of all available options, our hemorrhoid treatment in Dubai covers the full treatment pathway from conservative care to surgery. But not every symptom is caused by hemorrhoids — rectal bleeding can occasionally indicate something more serious. Getting a proper examination is the only way to know for certain.
This page explains the full range of hemorrhoid symptoms, what causes them, how internal and external hemorrhoids differ, and when you should see a specialist.
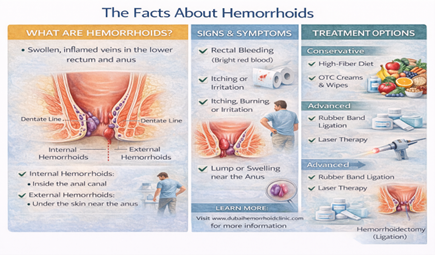
What Are Hemorrhoid Symptoms?
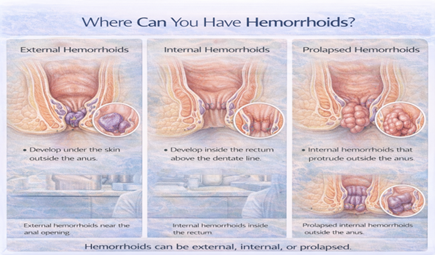
Hemorrhoids (also called piles) are swollen and enlarged blood vessels in the lower rectum and anal canal. The symptoms they cause depend entirely on their type and size.
Hemorrhoids are divided into two main categories:
⦁ Internal hemorrhoids — located inside the rectum, above the dentate line
⦁ External hemorrhoids — located under the skin around the anus, below the dentate line
Because these two types sit in anatomically different tissue, they produce very different symptoms. Internal hemorrhoids are usually painless but bleed. External hemorrhoids are often painful, particularly if a blood clot forms inside them.
Internal vs External Hemorrhoid Symptoms
Understanding which type of hemorrhoid you have is critical to determining the right treatment.
| Symptom | Internal Hemorrhoids | External Hemorrhoids |
| Bleeding | Bright red blood on paper or in toilet — common | Uncommon unless skin is broken |
| Pain | Usually painless (no pain receptors above dentate line) | Often painful, especially if thrombosed |
| Visible lump | Not visible unless prolapsed (Grade 3–4) | Visible or palpable lump outside anus |
| Itching | Common — mucus discharge irritates perianal skin | Common — skin irritation around anus |
| Prolapse | Possible at Grade 2–4 (tissue protrudes from anus) | Does not prolapse — it is already external |
| Thrombosis | Rare | Possible — sudden severe pain with hard purple lump |
If you are unsure which type you have, a clinical examination is the only reliable way to find out. A proper diagnosis takes approximately 5–10 minutes and is straightforward in experienced hands.
→ Related: Internal vs External Hemorrhoids in Dubai: Understanding the Difference
The Most Common Hemorrhoid Symptoms Explained
1. Rectal Bleeding
Bleeding is the most common symptom of internal hemorrhoids and the one that most often brings patients to my clinic. The bleeding is typically:
⦁ Bright red — not dark red or mixed with stool
⦁ Seen on toilet paper after wiping, or as a splash of blood in the toilet bowl
⦁ Not painful — internal hemorrhoids bleed without pain because rectal mucosa has no pain receptors
⦁ Occurs during or after a bowel movement, then stops
Bright red bleeding that stops quickly and is separate from the stool is usually hemorrhoidal. However, any rectal bleeding that is dark, mixed with stool, persistent, or accompanied by a change in bowel habit requires investigation to rule out colorectal polyps or cancer.
2. A Lump Near the Anus
- A palpable lump near the anus can have several causes:
⦁ External hemorrhoid — a soft or firm swelling under the perianal skin, present at rest
⦁ Thrombosed external hemorrhoid — a hard, painful, purple-blue lump that appeared suddenly
⦁ Prolapsed internal hemorrhoid — soft, moist tissue protruding from the anus, usually after straining
⦁ Skin tag — a painless flap of skin, often a remnant from a previous hemorrhoid
⦁ Perianal abscess — a tender, red, warm swelling that may be accompanied by fever
A lump combined with sudden severe pain almost always indicates a thrombosed external hemorrhoid or an abscess, both of which require prompt assessment.
3. Itching and Irritation Around the Anus
Persistent anal itching (pruritus ani) is one of the most uncomfortable hemorrhoid symptoms. It is caused by mucus leakage from internal hemorrhoids irritating the perianal skin, incomplete closure of the anal canal causing soiling, and skin tags trapping moisture. Itching also has non-hemorrhoidal causes including skin conditions and fungal infection, so if it does not respond to standard treatment, further evaluation is warranted.
4. Pressure, Heaviness or Feeling of Incomplete Evacuation
- Internal hemorrhoids can cause a persistent sensation of pressure, heaviness, or the feeling that you have not fully emptied your bowels. This is caused by the bulk of enlarged hemorrhoidal tissue inside the rectum. It is not dangerous but is a clear indication that treatment is required.
5. Pain
- Pain is not a primary symptom of uncomplicated internal hemorrhoids. If you have significant anal pain, the more likely causes are:
⦁ Thrombosed external hemorrhoid — sudden onset, severe, constant, worse on sitting
⦁ Anal fissure — sharp, tearing pain during and after a bowel movement, often with visible blood
⦁ Perianal abscess — throbbing constant pain with swelling, redness, and sometimes fever
If your main symptom is pain, do not assume it is a simple hemorrhoid. A fissure or abscess requires different treatment, and delaying care can worsen both conditions.
Mucus Discharge
- Enlarged internal hemorrhoids often produce a mucus discharge that causes soiling of undergarments and perianal skin irritation. Patients sometimes mistake this for incontinence. It is a specific sign of significant internal hemorrhoids and generally indicates that treatment beyond dietary modification is required
Why Hemorrhoids Bleed
Hemorrhoidal tissue is vascular — it consists of blood vessels that help control continence. When these vessels become enlarged and the supporting tissue weakens, the thin rectal mucosa covering them is vulnerable to trauma during bowel movements.
The passage of hard stool, straining, or even normal defecation can shear the surface of an internal hemorrhoid, releasing bright red arterial blood. This is why hemorrhoid bleeding is bright red (arterial, not venous), painless (the mucosa above the dentate line has no pain receptors), and usually self-limiting.
Chronic hemorrhoid bleeding, even if small in volume per episode, can over time contribute to iron deficiency anaemia. I have seen patients who had been bleeding for months, had become significantly anaemic, and had assumed the bleeding was normal or too minor to mention.
→ Related: Hemorrhoid Bleeding in Dubai: When to Worry and How to Get Properly Diagnosed
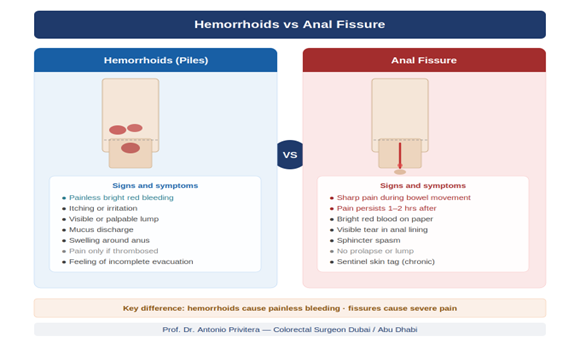
When Rectal Bleeding Is Not Hemorrhoids
This is the most clinically important section of this page. The symptoms of hemorrhoids — particularly rectal bleeding — overlap with symptoms of more serious conditions that require timely investigation.
You should not assume rectal bleeding is hemorrhoids if:
⦁ The blood is dark red or maroon, or is mixed in with the stool rather than separate from it
⦁ You have a change in bowel habit — looser stools, constipation, or pencil-thin stools for more than three weeks
⦁ You have unexplained weight loss
⦁ You have abdominal pain or cramping
⦁ You are over 45 with new rectal bleeding and have not had a recent colorectal screening
⦁ You have a family history of colorectal cancer or inflammatory bowel disease
⦁ Bleeding does not improve after four to six weeks of appropriate hemorrhoid treatment
Conditions that can mimic hemorrhoid symptoms include colorectal polyps, colorectal cancer, inflammatory bowel disease, diverticular disease, and anal cancer.
A proper examination — including digital rectal examination and anoscopy — takes less than ten minutes and will differentiate hemorrhoids from other causes. This is not optional when rectal bleeding is involved. It is essential.
If symptoms persist or are not improving, a specialist assessment in Dubai can help determine the most appropriate treatment.
What Causes Hemorrhoids?
Hemorrhoids develop when increased pressure on the veins of the lower rectum and anal canal causes the hemorrhoidal cushions to engorge, enlarge, and eventually lose their structural support. The most common contributing factors are:
Constipation and Straining
This is the primary driver. Straining to pass hard stool raises intra-abdominal pressure significantly, forces blood into the hemorrhoidal vessels, and over time weakens the connective tissue that holds them in place. Even a few minutes of straining per day, repeated over years, is enough to produce symptomatic hemorrhoids.
Prolonged Sitting — Particularly on the Toilet
Sitting on the toilet for more than a few minutes allows the anal sphincter to relax and hemorrhoidal tissue to engorge with blood. The unsupported position of the perineum on a toilet seat also increases venous pressure in the area. This is one of the most modifiable risk factors.
→ Related: Bathroom Habits That Prevent Hemorrhoids
Sedentary Lifestyle and Prolonged Sitting at Work
Office workers who sit for six to eight hours a day consistently present with higher rates of hemorrhoidal disease. Reduced physical activity slows bowel transit, increases constipation risk, and reduces pelvic blood flow.
→ Related: Why Dubai Office Workers Get Hemorrhoids More Often
Pregnancy
The growing uterus compresses the inferior vena cava, reducing venous return from the lower body and increasing pressure in the hemorrhoidal veins. Progesterone also slows bowel transit. Hemorrhoids are common in the second and third trimesters and immediately post-partum.
→ Related: Hemorrhoids During Pregnancy in Dubai: Safe Treatment
Low-Fibre Diet and Inadequate Hydration
A diet low in fibre produces small, hard, slow-moving stool that requires straining to pass. A high-fibre diet (25–35g per day) with adequate hydration is the single most effective dietary intervention for both preventing and managing hemorrhoids.
Heavy Lifting
Repeated heavy lifting raises intra-abdominal pressure sharply, with a similar effect to straining at stool. Correct breathing technique and avoiding breath-holding (Valsalva manoeuvre) during lifts reduces this risk.
Age
The connective tissue that supports hemorrhoidal cushions weakens with age. Symptomatic hemorrhoids are most common between ages 45 and 65, though they occur at any age.
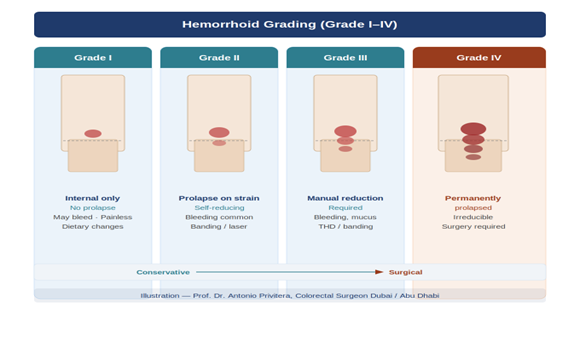
Hemorrhoid Grades and How Symptoms Progress
Internal hemorrhoids are classified by grade, which determines how they behave and what treatment is appropriate:
| Grade | What Happens | Main Symptoms | Typical Treatment |
| Grade 1 | Small internal swelling. Does not prolapse. | Painless bleeding; no visible lump | Diet, fibre, hydration |
| Grade 2 | Prolapse with straining; retracts spontaneously. | Bleeding; occasional prolapse after straining | Rubber band ligation; laser |
| Grade 3 | Prolapse requires manual reduction. | Bleeding; prolapse; mucus; pressure; itching | THD / rubber band ligation |
| Grade 4 | Irreducible prolapse. Cannot be pushed back. | Persistent prolapse; bleeding; soiling; discomfort | Hemorrhoidectomy |
→ Related: Grade 4 Hemorrhoids in Dubai: When Surgery Is Needed
When You Should See a Doctor
You should seek a clinical assessment if any of the following apply:
⦁ You have rectal bleeding for the first time — always investigate rather than assume
⦁ Bleeding persists for more than a few days despite dietary changes
⦁ You have sudden severe anal pain with a hard lump — possible thrombosed hemorrhoid (see within 48–72 hours)
⦁ You notice tissue protruding from the anus that you have to push back
⦁ You have persistent anal itching, mucus discharge, or soiling affecting daily life
⦁ You are over 45 with new rectal bleeding and have not had a recent colonoscopy
⦁ Home treatment has not worked after four to six weeks
⦁ You have fever, spreading redness, or pus near the anus — possible abscess, seek urgent care
A consultation for hemorrhoids is straightforward, dignified, and usually takes approximately 30 minutes including examination and discussion. The majority of patients leave with a clear diagnosis and a treatment plan on the same day.
Experiencing symptoms like these? A discreet same-day specialist assessment is available across Dubai.
WhatsApp: +971 55 318 8469 | Phone: +971 55 318 8469
Medcare Discovery Gardens (Dubai)
→ Related: When to See a Doctor for Hemorrhoids: Your Complete Guide
Treatment Options in Dubai
Treatment depends on the type of hemorrhoid, its grade, and the specific symptoms.
Conservative Management (All Grades)
⦁ High-fibre diet (25–35g per day) and increased fluid intake
⦁ Correct toilet habits — limit time on the toilet, avoid straining, consider a footstool
⦁ Topical treatments — creams or suppositories for symptom relief
⦁ Sitz baths for comfort
Rubber Band Ligation (Grade 1–3)
A small rubber band is placed at the base of the hemorrhoid, cutting off its blood supply. Performed in the clinic without anaesthesia, takes approximately five minutes, and most patients return to work the same day.
→ Related: Banding vs Laser vs THD for Hemorrhoids in Dubai
Laser Hemorrhoid Treatment (Grade 1–3)
A fine laser fibre shrinks the hemorrhoid from within. Precise, minimal post-procedure discomfort, well suited to patients concerned about pain.
→ Related: Laser Hemorrhoid Treatment in Dubai
THD — Transanal Hemorrhoidal Dearterialization (Grade 2–4)
A Doppler-guided procedure that locates and ties off the arteries supplying the hemorrhoid, causing it to shrink. No tissue excised. Associated with significantly less post-operative pain than conventional hemorrhoidectomy.
Hemorrhoidectomy (Grade 3–4)
Surgical excision under general or spinal anaesthesia. Reserved for large Grade 3 or Grade 4 hemorrhoids or cases where other treatments have failed.
→ Related: Hemorrhoids (Piles) Treatment in Dubai — Full Treatment Hub
This article is written and reviewed by Prof. Dr Antonio Privitera, consultant colorectal surgeon with fellowship training at Mayo Clinic (USA) and the Royal College of Surgeons (UK), specializing in hemorrhoid diagnosis and minimally invasive treatment.
Frequently Asked Questions
Can I have hemorrhoids without any bleeding?
Yes. External hemorrhoids often cause pain, itching, and a palpable lump without significant bleeding. Grade 1 internal hemorrhoids may bleed only intermittently. The absence of bleeding does not exclude hemorrhoids.
Is it normal for hemorrhoid symptoms to come and go?
Yes, this is typical, particularly for Grade 1 and Grade 2 internal hemorrhoids. Symptoms often worsen with constipation, dehydration, or prolonged sitting, and improve with dietary changes. Recurring symptoms are a sign the hemorrhoids are still present and should be treated.
Can hemorrhoid symptoms last for months or years?
They can, particularly if the underlying cause is not addressed. Hemorrhoids causing symptoms for more than four to six weeks without improvement, or that recur frequently, warrant clinical review and treatment.
Do hemorrhoids cause lower back pain or abdominal pain?
No. Hemorrhoids do not cause lower back pain or abdominal pain. If you have these symptoms alongside rectal bleeding or altered bowel habit, they should be investigated further.
Are hemorrhoid symptoms different in pregnancy?
The symptoms are similar — bleeding, discomfort, prolapse, itching — but may be more pronounced due to increased pelvic venous pressure. Most cases improve after delivery. Treatment during pregnancy focuses on conservative measures, though more active treatment is available if required.
Book a Consultation in Dubai
If you are experiencing any of the symptoms described on this page, the next step is a clinical examination. Hemorrhoids are one of the most common conditions I treat, and in most cases the diagnosis is clear and the treatment straightforward.
📱 WhatsApp (Fastest Response): +971 55 318 8469
📞 Phone: +971 55 318 8469
🌐 Book Online: dr-antonio.com/contact
Dubai Locations:
⦁ Medcare Medical Centre, Discovery Gardens
⦁ Medcare Women and Children Hospital
⦁ Medcare Royal Specialty Hospital
⦁ Clemenceau Medical Centre
⦁ Aster Hospital, Qusais
Same-day and emergency appointments available. All consultations are private and confidential.
Professor Dr. Antonio Privitera
Fellowship Training: Mayo Clinic | Royal College of Surgeons (UK)
European Board Certified in Colorectal Surgery